Acute Pancreatitis
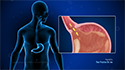
Acute pancreatitis is defined as inflammation of the pancreas that develops suddenly.
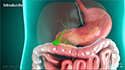
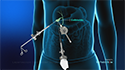
The pancreas is a vital gland, located behind the stomach just below the liver. It produces several digestive enzymes and also plays a vital role in maintaining blood glucose levels.
The pancreas is both an exocrine and an endocrine gland. The exocrine part produces enzymes that help in digestion and absorption of nutrients from food. The endocrine part of the pancreas secretes hormones involved in the metabolism of sugar and maintenance of blood sugar levels.
Disease Overview
In most cases, acute pancreatitis tends to be mild and resolves within a week or two. Symptoms may be worrisome for a few days, but then resolve, and the pancreas completely recovers. In some cases, however, acute pancreatitis can swiftly become severe and sections of the pancreas and surrounding tissues may undergo necrosis (tissue death). Pancreatic enzymes and chemicals may get into the bloodstream and cause inflammation and damage to other body organs. This can result in fatal complications, such as hypovolemic shock, kidney failure, respiratory failure, and other complications.
Causes
Acute pancreatitis is most often caused by gallstones or excessive intake of alcohol. Other causes may include:
- Injury or trauma to the pancreas
- Certain medications
- Infection
- Cystic fibrosis
- Blockage of the pancreatic duct or common bile duct
- Autoimmune diseases
- High calcium levels in the blood (hypercalcemia)
- High triglyceride levels in the blood (hypertriglyceridemia)
Risk Factors
Some of the factors that increase your chance of developing acute pancreatitis include:
- Family history of pancreatitis
- Diabetes
- Obesity
- Alcohol abuse
- Cigarette smoking
Signs and Symptoms
Acute pancreatitis is usually a milder form of pancreatitis, characterized by sudden and severe abdominal pain. Other symptoms include fever, vomiting, nausea, sweating, swelling in the abdominal region, a feeling of fullness due to gas, mild jaundice, and clay-colored stools.
Diagnosis
Your physician will review your symptoms and perform a physical examination of your abdomen. If certain areas are sensitive to touch, this may indicate acute pancreatitis. In addition, your physician may order laboratory tests that measure the levels of pancreatic enzymes, and imaging studies, such as a CT scan, MRI, or ultrasound, which can indicate inflammation of the pancreas and confirm the diagnosis.
Treatment
Treatment of acute pancreatitis is directed towards reducing the inflammation and treating the underlying cause of the condition. Mild cases may require hospital admission, where you will be given medication to manage pain, and intravenous fluids to prevent dehydration, which often accompanies pancreatitis. You will be closely monitored for recovery from your symptoms. Your doctor will stop food and fluids through the mouth to limit the activity of the pancreas. In severe cases, antibiotics may be administered, and surgery may be performed to remove the infected and damaged pancreas.
An endoscopic procedure called endoscopic retrograde cholangiopancreatography (ERCP) can be employed to aid in diagnosing and removing obstructions, such as gallstones in the bile duct and pancreatic duct, which may be causing your acute pancreatitis. Once there is improvement in your condition post treatment, you should completely avoid smoking, alcoholic drinks, and fatty foods.
Summary
Acute pancreatitis affects men more often than women. It typically resolves in a couple of days with treatment. A patient may need to undergo treatment in a hospital, depending upon the severity and the cause of the condition. Mild cases of pancreatitis improve with treatment, but severe cases can cause life-threatening complications. Therefore, if you experience symptoms of acute pancreatitis, it is important to seek medical care as soon as possible for early intervention.