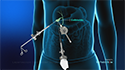
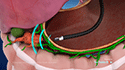
Colonic Stenting
Colonic stenting is a medical procedure in which a small, expandable, metal mesh tube called a stent is placed in the colon, also known as the large bowel or large intestine, to keep the colon open when it has become blocked (obstructed) or partly blocked by colon cancer or other forms of bowel blockage. The colonic stent is compressed tightly onto a small delivery wire which enables the stent to be placed across the tight narrowing, or area of blockage. Once expanded, it relieves the obstruction by keeping the bowel open. It can take about 24 hours for the stent to completely open after placement.
Indications
Your physician may recommend colonic stenting if your colon has become blocked and your bowel movements are unable to pass through it. This can result in bloating, pain or cramping, and sickness. A colonic stent can relieve these symptoms and restore proper colon function. Stents can be permanent or temporary. You may be offered a permanent stent to alleviate your symptoms if you cannot have surgery or if you choose not to have surgery. You may be offered a temporary stent if you wish to or are planning to have surgery to remove the cancer that is obstructing your bowel. By alleviating your symptoms, the stent provides you and your physician additional time to prepare for surgery. Some research indicates this can mean minimal time in intensive care or hospital and lead to fewer complications.
Preparation
Preparation for colonic stenting may involve the following steps:
- A thorough history and physical examination
- Routine blood work and imaging such as a CT (computed tomography) scan to see precisely where the blockage is located
- Informing your doctor of any medications or supplements you are taking or any conditions you have such as heart or lung disease
- Informing your doctor of any allergies to medications
- Refraining from medications such as blood thinners, aspirin, or NSAIDs, if indicated
- Refraining from solids or liquids at least 8 hours prior to the procedure
- Arranging for someone to drive you home after the procedure
Procedure
Colonic stenting is performed by specialist physicians; either by an interventional radiologist (utilizing special X-ray equipment) or by an endoscopist (utilizing a telescopic camera). These are commonly performed together. In general, the procedure involves the following steps:
- You will be brought to the X-ray department or an endoscopy suite.
- You will be asked to lie down on your side on the procedure table.
- An IV line is inserted into your arm to provide necessary medications and sedatives to keep you relaxed and ensure a comfortable procedure.
- Your physician will then insert a lubricated colonoscope through your rectum. Colonoscopes are tubes with a camera and a light at the end that are employed to examine the rectum, large intestine, and colon.
- You may feel slight cramping or pressure as the scope moves, but sedatives can help to reduce discomfort.
- Your endoscopist will advance the colonoscope to the narrowing in the colon and pass a soft wire (a guidewire) through the narrowing under X-ray guidance.
- Once the position of the guidewire is established, the narrow stent delivery system is passed through the colonoscope over the guidewire and across the stricture, or narrowing, under X-ray guidance.
- The constraining sheath is removed, and the stent will gradually expand over the next 24 hours to free the blocked colon and enable bowel contents to pass.
Post-procedure care
Following the procedure, you will be transferred to the recovery room where you will be closely monitored for the first 4 to 6 hours. You may have an X-ray 24 hours after your stent placement to see if it is in the correct position and has expanded properly. You may feel pain, soreness, or discomfort in the anal area due to the scope movement, as well as nausea or bloating. Medications are provided as needed to address these. A soft/pureed diet is recommended for the first few days. You should be able to resume your normal diet afterward unless your physician instructs otherwise. Stool softeners are also recommended to prevent fecal impaction within the stent if you have constipation. You may need to stay in the hospital for up to 48 hours to make sure your bowel is working properly again.
Risks and Complications
Colonic stenting is a relatively safe procedure, however, as with any procedure, some risks and complications may occur, such as:
- Bloating
- Nausea
- Rectal irritation
- Rectal bleeding
- Post-procedure pain
- Stent migration
- Bowel perforation (although this is very rare)
Summary
Colonic stenting is usually performed to relieve a complete or partial large bowel blockage often as part of treatment for cancer in that area. It is a safe and effective procedure that takes about 45 minutes to perform and offers significant relief from symptoms of bowel blockage, as well as helping to restore your normal bowel function.