Esophageal Stenting
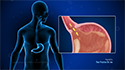
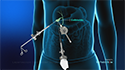
Esophageal stenting is a medical procedure in which a stent (a small plastic or metal tube) is placed into the esophagus (food pipe) to keep it open, enabling liquids and food to pass through into the stomach. The esophagus is a long tube through which food travels from the mouth down to the stomach. Narrowing or blockage of the tube can create problems with swallowing, a condition called dysphagia.
Disease conditions such as cancer of the esophagus can completely or partly block the tube and make swallowing difficult. Placing a stent into the blocked region opens the esophagus again, enabling you to swallow more easily.
Indications
Esophageal stenting is extensively utilized to treat a variety of conditions, most commonly esophageal dysphagia due to malignancy. Esophageal stenting is also used to treat esophageal strictures, perforations, leaks, and fistulas.
Preparation
Preparation for esophageal stenting may involve the following steps:
- A thorough history and physical examination
- Routine blood work and imaging
- Informing your doctor of any medications or supplements you are taking or any conditions you have such as heart or lung disease
- Informing your doctor of any allergies to medications or anesthesia
- Refraining from medications such as blood thinners, aspirin, or NSAIDs, if indicated
- Refraining from solids or liquids at least 8 hours prior to the procedure
- Arranging for someone to drive you home after the procedure
Procedure
Esophageal stent placement is usually performed under endoscopic and fluoroscopic guidance but can be performed with either modality safely. Most stents are placed distally and across the gastroesophageal junction, but proximal stent placement that requires more precise placement can also be performed.
The procedure may be done under conscious sedation or general anesthesia. If it is done under conscious sedation, you will receive medication to make you relaxed and sleepy. If it is done under general anesthesia, you will be asleep throughout the procedure.
During the procedure, your physician will first use an endoscope to look down your esophagus. An endoscope is a flexible tube with a powerful light source and camera on the end that is passed through your mouth and into the esophagus. If your physician notices any narrowing, they may need to widen or dilate it before stent placement. This is performed with soft, flexible, rubber tubes or special balloons passed through the endoscope.
Your physician will then place the stent under fluoroscopy guidance (real-time x-ray). After the stent is confirmed to be in the correct position, the rubber tubes or balloons are withdrawn so that only the stent remains in place.
Post-procedure care
Following the procedure, you will be transferred to the recovery room where you will be asleep or drowsy until the sedation or anesthesia wears off. You may feel pain, soreness, or discomfort in the throat once you gain consciousness. Pain and anti-nausea medications are provided as needed to address these. You should be able to take liquids once your anesthesia wears off and you no longer feel numbness in your throat. A soft or pureed diet is recommended for the first few days. You should be able to resume your normal diet in a couple of days unless your physician instructs otherwise. You may have to stay in the hospital for a day or two to ensure you can eat and drink comfortably before being discharged home.
Risks and Complications
Esophageal stent placement is a relatively safe procedure, however, as with any procedure, some risks and complications may occur, such as:
- Bleeding
- Throat soreness
- Stent migration
- Tumor growth into the stent
- Esophageal perforation
- Heartburn or acid reflux
Summary
Esophageal stenting is a procedure to place a small plastic or metal tube into the esophagus to treat esophageal narrowing or blockage. It is most commonly employed for symptomatic relief in those with swallowing difficulties secondary to malignancy. It is a simple and safe procedure that usually takes about 30 minutes and offers significant relief from symptoms of esophageal narrowing or blockage.