Polypectomy
A polypectomy is a surgical procedure to remove an abnormal mass of tissue called a polyp that develops on the inner wall of a hollow organ. A polypectomy is most commonly used to remove colon polyps.
Colon polyps are abnormal growths on the inner lining of any region of the colon. They may be cancerous or non-cancerous. Usually, the polyps grow and remain attached to the colon (benign tumor). Some polyps may begin to spread and invade other tissues in the body (malignant tumor).
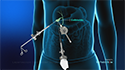
One or multiple colon polyps can be removed through open abdominal surgery, but more commonly this is performed during a colonoscopy. A colonoscopy is an endoscopic procedure used to view the large intestine (colon and rectum) using an instrument called a colonoscope (a flexible tube with a small camera and lens attached at one end) that is passed through the rectum. The endoscopist may snip off a small polyp with a forceps or remove a larger polyp with a snare that burns through the base of the polyp using channels in the colonoscope.
Indications
A polypectomy is indicated for removing polyps that may be causing symptoms, may be cancerous, or that require examination. Typically, a colonoscopy is first performed to detect the presence of any polyps. If any are detected, a polypectomy is performed at that time and the abnormal tissue is removed. The tissue is then sent for laboratory examination to determine if the growths are cancerous, precancerous, or benign. Colonoscopies can help to prevent colon cancer through early intervention.
Preparation for Polypectomy
Preparation for a polypectomy may include the following:
- Routine blood work and a review of your medical history.
- You should advise your doctor about any medications you are taking prior to the procedure.
- Inform your doctor if you are allergic to any medications or anesthesia.
- You may be prescribed laxatives or enemas to cleanse your bowel a day before the procedure.
- Do not eat or drink for at least 8-10 hours before the procedure.
- Arrange for someone to drive you home after the procedure.
Surgical Procedure
A polypectomy procedure is usually carried out at the same time as a colonoscopy and will involve the following steps:
- You will be placed on the operating table in a way that gives your physician the best access position to place the colonoscope.
- An IV line is started in your arm to administer anesthesia to make you sleep.
- Your vital signs such as heartbeat, blood pressure and respiratory function will be monitored.
- A colonoscope will be inserted into your rectum so your physician can view all segments of your colon.
- In addition to enabling visualization of the internal colon, the colonoscope allows your doctor to irrigate, suction, inject air, and access the intestine with surgical instruments.
- Your physician will remove any polyps (and possibly surrounding tissue) for further examination and possibly treat any other problems that are detected.
Post-Procedure Care
You will need to spend a couple of hours in the recovery room under observation while the anesthesia wears off. You may experience pain or discomfort in the rectum where the scope was passed through. Medications are provided as needed to address these. Your physician may ask you to avoid certain foods and drinks that can irritate your digestive system such as spicy foods, alcohol, coffee, tea, or soda for 2 to 3 days. You are advised to rest for a day or two before getting back to normal activities. A follow-up colonoscopy will also be scheduled to confirm that the polypectomy was successful and that no additional polyps have developed.
Risks and Complications
A polypectomy is a relatively safe procedure; however, as with any surgery, some risks and complications may occur, such as:
- Incomplete polyp removal
- Excessive bleeding
- Vomiting
- Irregular heartbeat
- Infection
- Severe abdominal bloating or pain
- Organ perforation
Summary
A polypectomy is a routine procedure to remove polyps and check for the presence of cancer. The main objective of the procedure is to establish whether the abnormal growth is cancerous, precancerous, or non-cancerous.