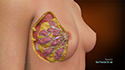
Axillary Sentinel Lymph Node Biopsy
When Breast cancer spreads to other parts of the body, it usually goes to the lymph nodes of the axilla or underarm. The sentinel lymph node is defined as the first node or group of nodes to which cancer cells are most likely to spread from a primary tumor. Axillary sentinel lymph node biopsy is a procedure to remove the sentinel lymph nodes in the axilla to examine them for malignancy.
Overview.
Lymph nodes are oval-shaped glands that contain cells that defend the body against foreign substances. They are part of the lymphatic system present in various parts of the body such as the neck, armpits, behind the ears, chest, abdomen and groin. The axillary sentinel nodes are the lymph nodes that first drain cancerous fluid from the breast. Usually there are between one and three sentinel nodes.
Indications.
Sentinel node biopsy is recommended for patients who have early breast cancer. Treatment for breast cancer usually involves removing some lymph nodes as well as removing the cancer from the breast. Testing the lymph nodes is very important, it gives you and your doctor information about the breast cancer and helps to plan further treatment.
Surgical procedure.
The sentinel node is identified, or ‘mapped' using a combination of two techniques:
Lymphatic mapping.
Blue dye test.
Lymphatic mapping is performed the day before, or a few hours before surgery. It is usually performed in a nuclear medicine or X-ray department. A small amount of radioactive material is injected either around the cancer or under the nipple. The radioactive tracer travels from the cancer site to the sentinel node, along the same lymphatic channels that cancer cells could travel. This can take a few minutes or a couple of hours. A series of pictures is taken to show where the sentinel node or nodes are located.
The skin over the sentinel node is marked with a pen. The injection of the tracer makes the sentinel node radioactive so it can be found by the surgeon with the use of a special probe during the operation. The dose of radiation is very small and will cause you no harm.
The blue dye test is performed at the beginning of the operation. When you are asleep, a small amount of blue dye is injected around the nipple or the tumor. The dye quickly moves into the lymphatic channels and turns the sentinel node blue, again helping the surgeon to locate the sentinel node.
Combining the blue dye and the radioactive technique helps your doctor identify sentinel lymph nodes very accurately.
Once the sentinel node is identified, a small incision is made and it is removed and sent to the laboratory for examination. If cancer cells are identified in the sentinel node, the biopsy is said to be positive. If this happens, your surgeon is likely to recommend you have an operation called an axillary clearance in which all the glands under your arm are removed. If cancer cells are not identified, the cancer is thought to be confined to the breast and may be treated by a wide local excision or a mastectomy.
Post-Operative Care.
Following the biopsy, you should keep your incision site dry for the first 24 hours. You may have some soreness and discoloration at the site due to the dye. Your doctor will prescribe pain medication to keep you comfortable. The discoloration will gradually fade away on its own.
Advantages & Disadvantages.
With a sentinel lymph node biopsy, fewer lymph nodes are removed resulting in less tissue damage. This minimizes complications and improves recovery time.
Risks and complications.
As with any procedure, sentinel lymph node biopsy may be associated with certain risks and complications such as pain, bruising, swelling, infection and nerve injury.
In the past when malignant breast cancer was identified, almost all axillary lymph nodes had to be removed, a very complicated procedure. With modern technology, the sentinel lymph node biopsy offers an alternative that is both accurate and easier for the patient to tolerate.