Benign Prostatic Hyperplasia
Benign prostatic hyperplasia (BPH), also referred to as benign prostatic hypertrophy, is the noncancerous enlargement of the prostate gland. It is the most common prostate problem in men as almost all men develop some degree of prostate enlargement as they age.
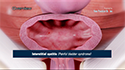
The prostate gland encircles the urethra, the tube that carries urine out of the body. When the prostate enlarges, it presses against the urethra, restricting urine flow through the tube and causing problems with urination and other associated symptoms.
Anatomy
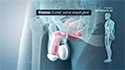
The prostate gland is a walnut-sized gland situated between the bladder and the penis, just in front of the rectum. It forms part of the male reproductive system and releases a fluid that protects and nourishes sperm. This fluid is secreted into the urethra and is discharged along with sperm as semen during ejaculation. The prostate is divided into 4 anatomical zones and enlargement typically occurs in the central and transitional zones of the prostate.
Causes
The exact cause of BPH is unknown. However, it is believed that factors connected to aging and changes in the cells of the testes may play a part in the growth of the gland, in addition to testosterone levels. Also, a family history of prostate issues or any abnormalities with your testes may increase your risk of prostate enlargement.
Signs and Symptoms
Symptoms are rarely seen before the age of 40, but over half of all men in their sixties and about 90% of men in their seventies and eighties show some symptoms of BPH, which may include:
- Frequent urination
- Straining to urinate
- Weak urine flow
- Inability to urinate
- Blood in the urine
- Pain with urination
- Loss of bladder control
- Incomplete bladder emptying
- Dribbling at the end of urination
- Delayed or slowed start to urination
Diagnosis
In order to diagnose BPH, your doctor may conduct the following tests and examinations:
- A review of your medical history and symptoms
- A digital rectal examination (DRE)
- A prostate specific antigen (PSA) blood test
- Urinalysis to check for infection or blood
- Urine flow study
- Prostate biopsy
- Bladder scans
- Post-void residual urine test
- Ultrasound
- Cystoscopy
Treatment
Conservative measures are always the first line of treatment for BPH. These measures may include the following:
- Watchful waiting: If you do not experience any symptoms of an enlarged prostate, your doctor may decide to use the wait-and-watch for the progression of the condition with regular monitoring and imaging studies, usually once a year.
- Medications: Medication is the most common treatment method for controlling symptoms of an enlarged prostate. There are a number of medications available, some which prevent growth of the prostate while others actually shrink it. Other drugs may be prescribed to improve urine flow and reduce bladder outlet obstruction.
Minimally Invasive/Invasive Treatment
The main objective of minimally invasive or invasive treatment is to reduce the size of the prostate gland and enlarge the urethra to make voiding easier. Treatment may include one of the following:
- Transurethral resection of the prostate (TURP): This involves removal of the part of the prostate causing the obstruction with the help of surgical instruments passed through the urethra.
- Transurethral incision of the prostate (TUIP): Incisions are made on the prostate with instruments introduced through the urethra to decrease the pressure on the urethra.
- Laser therapy: A laser is used to make cuts or destroy the obstructive part of the prostate.
- Transurethral needle ablation (TUNA): A heated needle is used to destroy part of the prostate.
- Transurethral microwave therapy (TUMT): This procedure involves using heat from microwave energy to destroy part of the prostate.
- UroLift: A new system which uses implants to lift and hold the enlarged prostate tissue away from the urethra.
- Open prostatectomy: This involves making an incision on the skin to access and remove the prostate. This is rarely used and mostly recommended for very large prostates.
Risks and Complications of Surgery
Some of the risks and complications of prostate surgery may include:
- Urinary tract infections
- Blood in the urine
- Erectile dysfunction
- Retrograde ejaculation
- Urinary incontinence
- Sudden inability to urinate
- Damage to surrounding tissues or organs
- Recurrence of prostate enlargement
Summary
It is common for the prostate gland to become enlarged as men age. It is important to discuss your symptoms of an enlarged prostate with your physician, no matter how minor you feel they may be. Your physician will work with you to develop a treatment plan that helps you manage your symptoms and lead a healthy life.