Prostate Biopsy
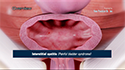
The prostate is a small, walnut-shaped gland that is only present in men. It is involved in providing nutrition to sperm and assisting in their transport.
A prostate biopsy involves the removal of small samples of suspicious tissues from the prostate.
Prostate biopsy is recommended when the results of initial tests, such as prostate-specific antigen (PSA) blood test or digital rectal exam (DRE), raise concerns of possible cancer.
The biopsy procedure is performed by a urologist. During the procedure a fine needle is used to collect tissue samples from the prostate gland.
After the tissue samples are obtained, they are examined under a microscope for cell abnormalities which may denote prostate cancer. Biopsy also helps in evaluating the stage and type of cancer to assist the doctor in formulating the most appropriate treatment option.
Indications for prostate biopsy.
A prostate biopsy is employed for early detection of prostate cancer, it is recommended under the following circumstances:
The prostate-specific antigen (PSA) blood levels are higher than normal.
Abnormal findings are detected during digital rectal exam.
High prostate-specific antigen (PSA) levels even after a normal biopsy.
Presence of non-cancerous abnormal cells in previous biopsy.
Types of prostate biopsy procedures.
There are different ways prostate biopsy samples can be collected. The most common techniques include:
Transrectal technique in which the needle is passed through the wall of the rectum.
Transurethral technique where the tissue sample is collected through the urethra. This procedure employs a long, thin tube set with a camera to approach the prostate.
Another common procedure used for a prostate biopsy involves insertion of the needle through the perineum, the skin between the anus and scrotum. This procedure requires a small incision in the perineum through which the biopsy needle is inserted.
Transrectal prostate biopsy procedure.
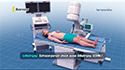
Transrectal prostate biopsy is the most common procedure employed by urologists. During this procedure the patient is placed on their side with their knees pulled up against the chest. In some cases, patients may be asked to lie on their stomachs.
The area around the anus is cleansed and lubricant is applied to enable smooth insertion of the ultrasound probe into the rectum.
Images are generated with the help of transrectal ultrasonography to assist the urologist in guiding the biopsy needle to the prostate.
Local anesthesia is given to reduce the discomfort related with prostate biopsy.
After proper positioning of the biopsy device, thin, cylindrical sections of tissue are obtained with a hollow, spring-propelled needle.
Usually about 10 to 12 tissue samples are obtained.
This may cause an unpleasant sensation for a short period of time while the samples are being taken. The procedure is usually completed in 5 to 10 minutes.
Post-operative care.
After the procedure, patients are prescribed antibiotics to prevent infection. You may notice small amounts of blood in your urine, stools or semen that should resolve in a few weeks. However, consult your doctor immediately in case of prolonged, heavy bleeding, exaggeration of pain, swelling or difficulty urinating.
Risks and complications
Risks factors associated with a prostate biopsy include infections, bleeding and difficulty urinating.
Some patients may develop a urinary tract or prostate infection which can be managed with antibiotics.
Bleeding at the biopsy site is common so patients should abstain from blood-thinning medications for a specified period as advised by the doctor.
Following a prostate biopsy a few patients may notice blood in the semen. This may continue for from 4 to 6 weeks and is not a matter of concern.
In some cases, the patient may have difficulty in passing urine. In such cases a temporary urinary catheter can be inserted.
Prostate biopsy is a diagnostic procedure conducted by a urologist to evaluate a patient for prostate cancer. Transrectal prostate biopsy is the most common approach performed by urologists. It is a relatively safe procedure with minimal complications.