Psoriatic Arthritis
Psoriasis is an autoimmune disease where the body’s own immune system attacks the skin causing scaly red and white patches to develop. Some people with psoriasis develop a type of arthritis called psoriatic arthritis, where their immune system also attacks the body’s joints, causing pain and inflammation. Some individuals experience a stable mild form of the disease whereas others experience severe symptoms that require long-term therapy.
Types.
Based on the location of the affected joints in the body and specific symptoms, psoriatic arthritis can be classified into five types:
Symmetric arthritis usually affects the same joint on both sides of the body.
Asymmetric arthritis involves one to three small or large joints in the body such as the hip, knee and fingers.
Distal interphalangeal predominant psoriatic arthritis affects the finger and toe joints closest to the nailbed.
Spondylitis is inflammation in the spinal column causing symptoms such as stiffness in the neck, lower back, or the pelvic area.
Arthritis mutilans is an rare destructive type of psoriatic arthritis that affects the distal joints of the fingers and toes and also causes neck or lower back pain.
Causes.
The exact cause of psoriatic arthritis is not known. It occurs when your body’s immune system attacks the healthy cells, inflames the joints and increases the production of skin cells. Various reasons for triggering the immune system include:
Family history of psoriasis or psoriatic arthritis
Environmental factors such as physical trauma, and viral or bacterial infection.
Obesity.
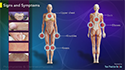
Signs and Symptoms.
The signs and symptoms of psoriatic arthritis include:
Painful, swollen joints in the fingers and toes (Dactylitis).
Joint inflammation between the vertebrae of the spine (Spondylitis).
Pain, swelling and tenderness in the regions where the tendons and ligaments attach to the bones such as the foot, heel, hip, knee and chest (Enthesitis).
Morning stiffness and fatigue.
Reduced joint range of motion.
Eye inflammation.
Nail changes such as pitting, discoloration, and thickening.
Finger or toe nail detachment.
Diagnosis.
The doctor will review your family history and examine your joints and skin for signs of psoriatic arthritis.
The physical examination includes looking for swelling and inflammation of the joints, signs of psoriasis on the skin or changes in the fingernails and toenails.
Your doctor will order tests to rule out rheumatoid arthritis or gout. Diagnostic tests include:
Imaging tests such as X-rays to detect changes in joints and MRI to check for problems with tendons and ligaments.
Blood tests for examining indicators of inflammation such as C-reactive protein and rheumatoid factor.
Joint fluid test involves removing a small sample of fluid from the affected joint to analyze for the presence of uric acid crystals to rule out gout.
Treatment.
Although there is no cure for psoriatic arthritis, symptoms can be managed. Treatment is focused on controlling joint inflammation and psoriatic patches on the skin, preventing joint damage and preserving joint function.
Your doctor will prescribe medications for managing the symptoms and inflammation of psoriatic arthritis. Different classes of medications include:
Nonsteroidal anti-inflammatory drugs or NSAIDs to relieve pain and reduce inflammation.
Disease-modifying anti-rheumatic drugs to slow the progression of the disease and protect the joints and tissues from permanent damage.
Immunosuppressants to suppress your immune system.
TNF-alpha inhibitors to inhibit stiffness, pain, tenderness and swelling.
Antibiotics to treat or prevent infection.
Steroid injections may be recommended to reduce inflammation and pain of the affected joint.
Creams or ointments may be prescribed to treat the psoriatic skin patches. If the condition does not improve with topical medications, your doctor may advise you to undergo phototherapy which exposes your skin to high-intensity ultraviolet light.
Occasionally, your doctor may suggest joint replacement surgery for repairing the damaged tendons and joint. The damaged part is replaced with a metallic or plastic artificial prosthesis.
Psoriatic arthritis is a chronic condition which leads to permanent joint damage if not treated in a timely fashion. Psoriatic arthritis may be confused with other conditions such as gout or rheumatoid arthritis, thus a proper diagnosis is essential for prescribing the most appropriate therapy. Talk to your rheumatologist if you have any concerns regarding psoriatic arthritis.