Systemic Lupus Erythematosus
A healthy immune system helps our body to fight off infections and disease such as cancer by making protective antibodies that attack these foreign invaders in the body. Sometimes, the immune system doesn't work properly and instead of attacking foreign invaders, it attacks our own tissues. This is referred to as an auto immune disorder.
SLE is a chronic auto-immune disease characterized by the formation of auto antibodies that attack the body’s own tissue causing damage to various organs and tissues. SLE can affect tissue anywhere in the body but it mainly affects the joints, kidneys and skin. The disease can affect all ages but is more common in people between 20 and 45 years of age. It occurs 10 x more often in women than men and is also more common in blacks and Asians.
Cause.
The precise reason why the immune system misfires is not clear but genes seem to play an important role in determining susceptibility to the disease. Thus, the presence of autoimmune diseases such as lupus, rheumatoid arthritis, diabetes or autoimmune thyroid disorders in the family history increases the risk of developing SLE.
Often, an environmental factor such as an infection, exposure to sunlight or drug allergies acts as a trigger and the body starts producing auto-antibodies against its own tissue. These antibodies are mostly antinuclear antibodies (ANA) that react with the body's own DNA leading to the formation of immune complexes that deposit on blood vessel walls, in joints and internal organs like kidneys, stimulating a severe inflammatory reaction that damages the tissue.
Symptoms and diagnosis.
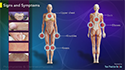
The symptoms of SLE depend on the body part affected. General symptoms may include fever, fatigue, weight loss, blood clots, hair loss in spots or around the hairline, heartburn, stomach pain and poor circulation to the fingers or toes. Pregnant women may even have a miscarriage.
The symptoms vary from person to person and may also come and go, suddenly. This makes the diagnosis of SLE difficult. The rheumatologist will perform a physical examination and will listen for an abnormal heart sound called a heart or pleural friction rub with a stethoscope. A nervous system examination will also be done. The rheumatologist will also look for typical signs of the disease that include:
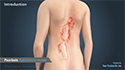
Rashes: The rash may occur as a simple rash on skin exposed to the sun, a round or disc shaped red raised rash with scales (discoid rash) or butterfly shaped rash over the cheeks (malar rash).
Mouth sores: The sores may be present in the mouth or nose and may last a few days to more than a month.
Arthritis: Swelling and tenderness may occur in two or more joints and may last for a few weeks.
Lung inflammation (pleuritis) or heart inflammation (pericarditis):These may cause chest pain when taking a deep breath.
Poor kidney function: This may be reflected in the presence of blood or protein in the urine.
Neurologic problems: such as seizures, strokes or psychosis.
If the rheumatologist finds at least four of these problems present and cannot find a valid reason for them, the rheumatologist may suspect SLE. To confirm the suspicion, the rheumatologist may order a series of blood screening tests. Antinuclear antibody (ANA) test is the most important test among these.However, a positive ANA does not necessarily indicate SLE. Therefore, more specific tests such as anti-double strand DNA, anti-smith or anti-phospholipid antibodies may also be ordered. Complement proteins may also be measured to detect or check the progression of the disease.
Treatment.
There is no cure for SLE. Treatment is aimed at managing the symptoms and providing the best quality of life for the patient. Patients with mild SLE are treated conservatively with non-steroidal anti-inflammatory drugs and anti-malarial drugs.Corticosteroid creams may be prescribed to treat skin rashes. For patients with serious life threatening symptoms indicating central nervous system, heart, lung or kidney involvement, aggressive treatment is given with high dose corticosteroids and immune-suppressants. If the symptoms do not improve or get worse, cytotoxic drugs may be prescribed.
Conclusion.
SLE is a very complex disease. It has many symptoms and is difficult to diagnose. There is no cure for SLE but with improvements in treatment most people with SLE can live active normal lives. Since SLE can flare up or go into remission suddenly, frequent heath checkups are essential to track the symptoms and change the treatment as needed.