Juvenile Arthritis
Arthritis is a chronic inflammatory disease-causing pain, swelling, and stiffness in the joints and may restrict the movements of limbs. Juvenile arthritis is the term used to describe arthritis in children younger than 16 years.
Juvenile arthritis is twice as common in girls than boys and the most common type is juvenile idiopathic arthritis (JIA). Juvenile idiopathic arthritis is an autoimmune disorder affecting the joints of the knee, hands and feet. It causes pain, swelling, stiffness, and feeling of warmth in the joints.
Causes The probable causes of juvenile idiopathic arthritis include:
Autoimmune condition: This is a disorder in which the child’s immune system fails to recognize the body’s own tissues, the synovial cells in the joint, causing the body to attack and destroy the cartilage and bone. The reason for this condition is unknown.
Genetic factors: It is believed that some of the genes inherited by the child from the parents may increase the risk of developing juvenile arthritis.
Environmental factors: A viral infection can trigger the disease.
Signs and Symptoms
The most common symptoms of juvenile arthritis are pain and swelling in the joints with joint stiffness that may worsen in the morning or after bedtime.
Other symptoms include:
Restricted movements of the affected joint causing your child to limp in the morning.
Fever or a skin rash if your child has systemic juvenile arthritis.
Swollen lymph nodes of the neck or other areas of the body.
Types of Juvenile Arthritis
Juvenile idiopathic arthritis is a group of arthritic disorders and is classified by the International League of Associations for Rheumatology (ILAR) into seven types based on the characteristic symptoms.
Systemic arthritis
Oligoarthritis (pauciarticular juvenile rheumatoid arthritis)
Polyarthritis – rheumatoid factor positive
Polyarthritis – rheumatoid factor negative
Psoriatic arthritis
Enthesitis-related arthritis
Undifferentiated arthritis
Systemic arthritis
Systemic arthritis was formerly called systemic juvenile rheumatoid arthritis. The child may have intermittent fever for 2 weeks before or along with symptoms of arthritis. The fever may be high for at least 3 days. Fever and arthritis symptoms may be accompanied by other signs such as enlarged lymph nodes, liver, or spleen; inflammation of the membrane lining the heart or lungs; characteristic rheumatoid rash, a pale pink rash that may last for a few minutes or hours and then disappear.
Oligoarthritis
Oligoarthritis was formerly called pauciarticular juvenile rheumatoid arthritis. In this form of arthritis, one to four joints may be affected during the first 6 months of this disease. This is further divided into two sub-categories based on the number of joints involved:
Persistent oligoarthritis – Not more than four joints get affected at any time during the course of the disease.
Extended oligoarthritis – More than four joints get affected after 6 months.
Polyarthritis
Polyarthritis was earlier known as polyarticular rheumatoid arthritis and the two sub-variants are rheumatoid factor negative and rheumatoid factor positive.
The child may have arthritis in five or more joints in the first 6 month period of the disease. When the test for rheumatoid factor remains negative it is polyarthritis rheumatoid factor negative. If two tests done at 3 month intervals are positive, it is diagnosed as polyarthritis rheumatoid factor positive.
Psoriatic arthritis
In this type. arthritis coexists with a skin condition called psoriasis or with any two of these conditions:
Dactylitis (swelling of the finger or toe because of inflammation)
Nail pitting or splitting
Family history of psoriasis
Psoriasis is an autoimmune inflammatory skin condition characterized by thick, red skin with silver-white patches called scales.
Enthesitis-related arthritis
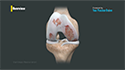
This type of arthritis is accompanied with enthesitis which is inflammation at the site where the ligament, tendon or joint capsule joins the bone. Enthesitis occurs most commonly around the knees and at the Achilles tendon on the back of the ankle.
Diagnosis Your doctor will carefully examine your child for symptoms and collect medical and family history. In addition, some diagnostic tests may be required to confirm the disease and disease sub-type. These include:
Blood tests: Blood is tested for anti-cyclic citrullinated (CCP) antibodies, rheumatoid factor, antinuclear antibodies, and erythrocyte sedimentation rate (ESR). Blood tests help to identify the type of juvenile arthritis and to rule out other diseases.
X rays: X-rays may be required to confirm any injury to the bone or unusual bone development.
Differential diagnosis: Certain other tests may be performed to exclude other conditions such as viral infections and physical injuries that may have similar symptoms to arthritis.
The treatment for juvenile arthritis is aimed at reducing the symptoms such as swelling and pain in the joints and preventing further complications. A combination approach of both medicine and physical therapy helps to improve the physical activities of your child.
Medications:
Nonsteroidal anti-inflammatory drugs: Nonsteroidal anti-inflammatory drugs (NSAIDs) relieve the joint pain and swelling by blocking the substances that cause inflammation. These are the first line of medications prescribed.
Disease-modifying antirheumatic drugs (DMARDs): These drugs are often prescribed along with NSAIDs to reduce pain, stiffness, and inflammation and slow down the progression of the disease.
Corticosteroids: Corticosteroids are prescribed in moderate to severe cases of juvenile arthritis with inflammation of the heart sac, pericarditis, or for acute stages of arthritis. They are available as oral medications or in the form of injections. When only one or a few joints are affected, corticosteroid injections are recommended to provide quick relief from pain in the joint.
Biologic agents or biologic response modifiers: These medications act by blocking the tumor necrosis factor (TNF) that causes inflammation.
Physical therapy: Physical therapy programs involve a regular schedule of exercises added to your child’s treatment plan. Physical therapy helps to improve muscle tone and recover the motion of the joints. The use of splints may be recommended to guide normal growth of the bone and joints.
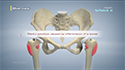
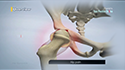
Surgery: Surgical intervention is usually not needed, but in severe cases of polyarticular juvenile arthritis, joint replacement surgery of the hips may be considered after bone growth is complete. Surgical correction may also be needed in conditions of marked leg length variations.