Latarjet Procedure
The shoulder joint provides a wide range of movement to the upper extremity, but injuries or repeated dislocations can cause instability to the joint. The Latarjet procedure is a surgical procedure performed to treat shoulder instability by relocating a piece of bone with an attached tendon to the shoulder joint.
Disease Overview
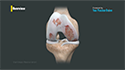
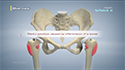
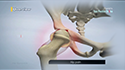
The shoulder joint is a ball-and-socket joint with the head of the humerus (long arm bone) forming the ball, and a cup-shaped depression on the shoulder blade (glenoid fossa) forming the socket.
The joint is stabilized by the labrum, a cartilaginous rim of the glenoid cavity, and the capsule, a series of ligaments that enclose the joint. Injury and trauma can tear or stretch the labrum and/or ligaments, causing instability and dislocation of the joint. The shoulder can dislocate in front (anterior), down (inferior) or behind (posterior), but anterior dislocation is the most common. Tearing of the labrum due to trauma is called a Bankart tear, which sometimes involves the breaking of bone along with the labrum. This is referred to as a bony Bankart tear. Shoulder instability can lead to pain and a feeling of giving way.
Indications
The Latarjet procedure is indicated for anterior shoulder instability that is recurrent and caused by large bony Bankart lesions, especially if there is a Hill-Sachs lesion. The Latarjet procedure is considered when this type of damage could not be repaired with a labral repair alone.
Surgical procedure
The Latarjet procedure is performed under general anesthesia with the patient in a semi-reclined or beach-chair position.
- An incision of 5 cm is made from your shoulder blade towards the armpit.
- Retractors are used to separate the muscles of the shoulder and chest and expose the coracoid process (a small, hook-like structure of the shoulder bone) and its attached tendons.
- The coracoid process is freed of its attachments and along with the conjoined tendon is transected from its base.
- Holes are drilled into the transected coracoid process.
- The subscapularis muscle, which passes in front of the shoulder joint is split in line with its fibers.
- The capsule of the shoulder joint is entered and the glenoid is exposed in order to receive the coracoid.
- The transected coracoid with the conjoined tendon is passed through the separated subscapularis muscle and fixed to the glenoid rim with screws. This increases the glenoid surface and stabilizes the joint. The conjoined tendon and subscapularis muscle provide additional stability by acting as a sling.
- Upon completion, the instruments are withdrawn, and the incision is closed and covered with a sterile bandage.
Post-Operative Care
Following the procedure your arm is placed in a sling to rest the shoulder and promote healing. You may remain in the hospital the night of the surgery before being discharged home. Pain is controlled with medication and ice packs. You will be instructed to keep the surgical wound dry and to wear your sling while sleeping for a few weeks after the procedure. The sling may be removed in 3 to 6 weeks.
Rehabilitation usually begins early on the first postoperative day with finger movements and passive assisted range of motion exercises. A physical therapy program is recommended for 3 months after which you can return to your regular activities.
Risks and complications
The Latarjet procedure usually provides good results, but as with all surgical procedures, complications can occur, and include:
- Hematoma (bleeding)
- Fracture or failure of union of the coracoid.
- Stiffness due to inadequate rehabilitation
- Recurrence of instability and infection – although these are rare
Summary
The Latarjet procedure is successful in treating shoulder instability due to bone loss or laxity with minimal recurrence. Adequate physical rehabilitation is necessary for you to return to your regular activities early and without complications.