Medial Patellofemoral Ligament (MPFL) Reconstruction
Medial patellofemoral ligament (MPFL) reconstruction is a surgical procedure used to treat patellar instability, particularly in cases where the patella (kneecap) dislocates (luxates) or partially disclocates (subluxates).
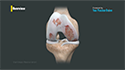
The patella is a protective bone attached to the quadriceps muscle of the thigh by the quadriceps tendon. The patella attaches with the femur (thighbone), forming the patellofemoral joint. The patella is protected by the medial patellofemoral ligament which prevents the kneecap from gliding out of alignment. The MPFL is a key ligament that stabilizes the patella, keeping it aligned with the femur as the knee bends and straightens.
Indications
Your surgeon may recommend medial patellofemoral ligament (MPFL) reconstruction in the following scenarios:
- Recurrent patellar dislocations or subluxations.
- Severe patellar instability that has not responded to conservative treatments like physical therapy or bracing.
- Damage to the MPFL due to trauma or injury.
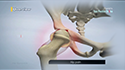
Dislocation of the patella occurs when the patella moves out of the patellofemoral groove, (called the trochlea) onto the bony head of the femur. If the kneecap partially comes out of the groove, it is called subluxation, and if the kneecap completely comes out, it is called luxation (or more commonly, dislocation) Patellar dislocation is often observed in athletes around 15 to 20 years old, and commonly affects women because of their wider pelvis, which creates a lateral pull on the patella.
Some of the causes for patellar dislocation include a direct blow or trauma, twisting of the knee while changing direction, muscle contraction, and congenital defects. It also occurs when the MPFL is torn. Common symptoms include pain, tenderness, swelling around the knee joint, restricted movement of the knee, numbness below the knee, and discoloration of the area where the injury has occurred.
Preparation
Preoperative preparation for MPFL reconstruction includes:
- A comprehensive medical evaluation, including physical examination, blood testing, and imaging studies
- Informing your doctor of any allergies to medications, anesthesia, or latex
- Providing your physician with a list of any medications or supplements you are taking
- You may need to adjust or temporarily stop taking certain medications - especially those that can affect blood clotting
- Disclosing any recent illnesses or other medical conditions you may have
- Stopping smoking, as it can negatively impact the healing process and increase the risk of complications
- Abstaining from food or drink for at least 8 hours prior to surgery
- Signing an informed consent form
Surgical procedure
In general, MPFL reconstruction surgery may include the following steps:
- The patient is typically placed under general or regional anesthesia.
- The patient is positioned supine (lying on the back) with the affected knee slightly flexed, allowing easy access to the surgical area.
- A small incision is made on the inside of the knee to harvest the selected graft tendon.
- A graft is usually harvested from the patient’s hamstring tendons, such as the gracilis or semitendinosus tendon.
- The harvested tendon is then prepared to be used as the new MPFL. In some cases, an allograft (donor tissue) may be used.
- Small incisions are made to create tunnels in the femur and patella. These tunnels will hold the graft in place.
- The graft is passed through the tunnels and secured at both ends using fixation devices such as screws or anchors. The graft is tensioned to ensure proper alignment and stability of the patella.
- The incisions are closed, and the knee is bandaged.
Postoperative care
After the surgery, the knee is usually immobilized in a brace for a few weeks to facilitate healing and protect the treated area. Initial recovery includes rest, ice, compression, and elevation (RICE), as well as limited weight-bearing with crutches. Pain medications are provided as needed. Rehabilitation begins shortly after surgery to restore range of motion, strength, and stability to the knee. Patients can usually return to sports or full activity within 6-12 months, depending on their recovery progress. Follow-up appointments will be scheduled to monitor your progress and adjust the rehabilitation program as needed.
Risks and Complications
As with any surgery, some risks and complications may occur, such as:
- Infection
- Bleeding
- Blood clots or deep vein thrombosis (DVT)
- Graft failure
- Persistent instability or stiffness in the knee
- Hardware complications
- Anesthesia-related risks
Summary
MPFL reconstruction is a highly effective procedure for addressing recurrent patellar dislocations, with a high success rate in restoring stability to the knee.